

About Company
Brief About RCM Advisors
At RCM Advisors, we specialize in providing comprehensive Revenue Cycle Management solutions to streamline your financial processes and optimize revenue capture. Our tailored services address key pain points such as:
- Billing Accuracy
- Workflow Efficiency
- Compliance Assurance
- Revenue Optimization
Understanding Your Pain Points
Several pain points can arise in the RCM process for hospitals, impacting their financial health and operational efficiency. Here are some common pain points
- Claim Denials
- Billing Errors
- Inefficient Coding Processes
- Insurance Verification Challenges
- Patient Collections
- Regulatory Compliances
- Integration Issues
- Delayed Reimbursements
- Staff Training and Turnover
- Incomplete or Inaccurate Documentation

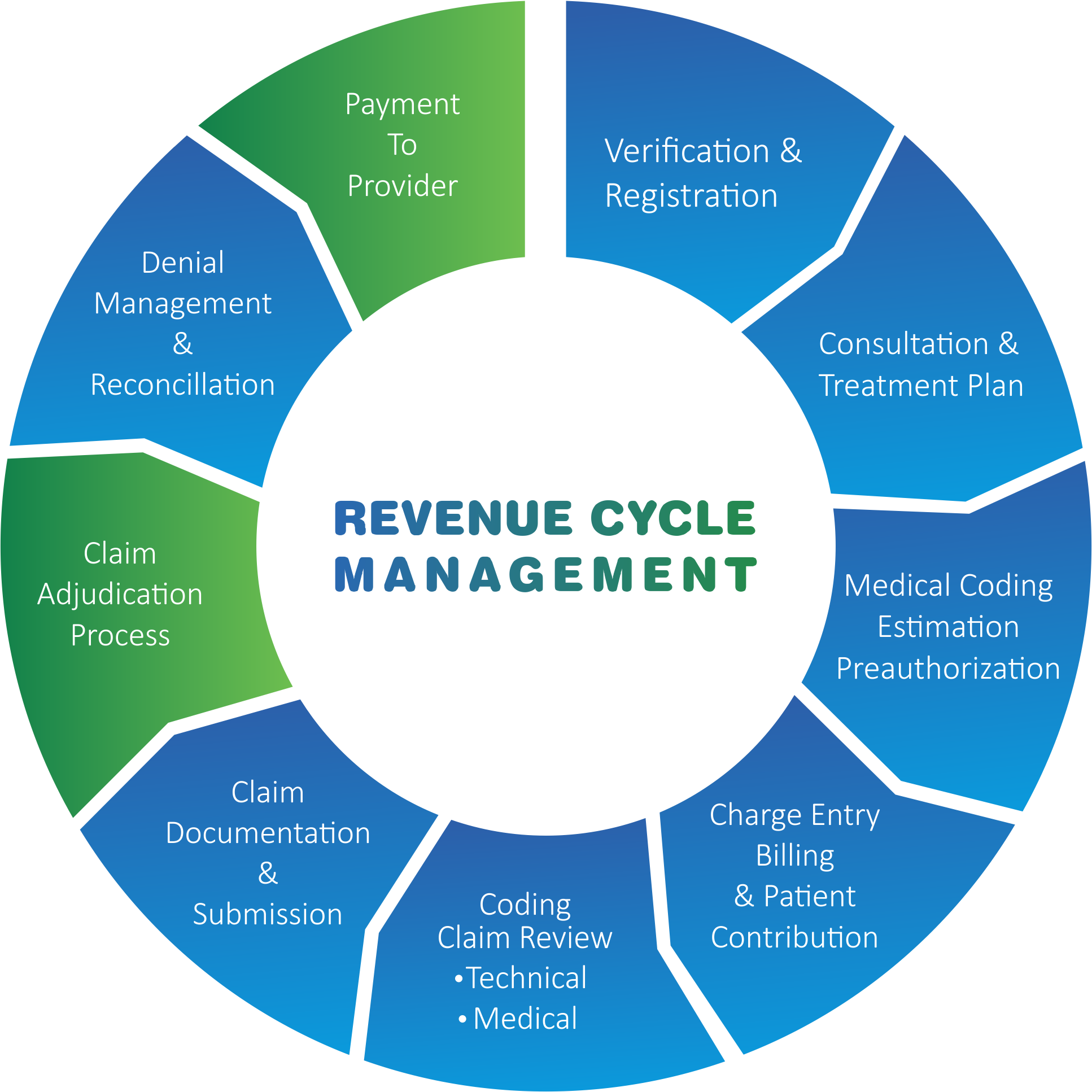
Our Comprehensive RCM Solutions
Comprehensive Revenue Cycle Management (RCM) solutions aim to address the various challenges and pain points faced by hospitals and healthcare providers in managing their financial processes effectively. Here are key components and features of a comprehensive RCM solution.
Read MorePowered By Innovation
RCM is critical aspect of healthcare and various technology tools have been developed to streamline and optimize the financial processes associated with patient care. These tools helps healthcare providers manage everything from patient registration and insurance verification to billing and collections. Here are some innovative technology tools used in RCM:
- EHR and EMR Systems
- Patient Access Solutions
- Claims Processing and Management
- Revenue Integrity Solutions
- Data Analytics and Business Intelligence
- Patient Financial Engagement Tools
- Payment Processing Solutions
- Blockchain Technology
- Robotic Process Automation
- Telehealth Solutions
- Compliance Management Systems
- Artificial Intelligence for Predictive Analytics


Ensuring Compliance And Mitigating Risks
Commitment to regulatory compliance is crucial in healthcare industry due to the complex and highly regulated nature of healthcare finance. Here are some key ways in which healthcare organizations can demonstrate commitment to regulatory compliance in the context of RCM:
- Adherence to Healthcare Regulations
- Comprehensive Training Programs
- Utilization of Compliance Management Systems
- Data Security and Privacy Measures
- Documentation and Record Keeping
- Monitoring and Reporting
- Engagement with Regulatory Bodies
- Regular External Audits and Assessments
- Collaboration with Payers and Partners
- Technology Solutions for Compliance
- Continuous Improvement Culture
Our Performance Metrics
We follow - MGMA standards are a set of metrics used to determine the overall performance of medical practice in the United States. These metrics are actually the key indicators for practice performance success. The interpretation of these MGMA benchmarks is essential to assess the overall practice performance.
MGMA DataDive is an industry-wide data set that includes thousands of metrics that you can use to benchmark almost any area of your practice.
| Departments | Metrics | Benchmarks |
|---|---|---|
| Billing | Rejection % | 2% - 3% |
| Charge Lag | 2% | |
| Rejection TAT | 2 Days | |
| Payments | Collections % | 100% |
| Denials % | 4% of total charges billed in month | |
| Payment posting TAT | 2 Days |
| Departments | Metrics | Benchmarks |
|---|---|---|
| AR | AR Pat % | 3% of Total Outstanding AR |
| AR Ins 0-30 Days | 40% | |
| AR Ins 31-90 Days | 20% | |
| AR Ins 91-120 Days | 15% | |
| AR Ins 121-151 Days | 10% | |
| AR Ins 151-180 Days | 8% | |
| AR Ins 181-365 Days | 5% | |
| AR Ins 365+ Days | 2% |
Maximizing Revenue Potential
Maximizing revenue potential in RCM is critical for healthcare organizations to ensure financial sustainability and provide quality patient care. Here are strategies to optimize revenue potential in RCM
- Enhance Patient Access and Registration
- Streamline Claims Processing
- Claims Processing and Management
- Optimize Coding Accuracy
- Improve Charge Capture
- Utilize Revenue Cycle Analytics
- Automate Prior Authorization Processes
- Patient Financial Engagement
- Implement Price Transparency
- Enhance Denial management
- Optimize Revenue Integrity
- Implement Technology Solutions
- Staff Training and Education
- Optimize Contract Negotiations


